
For more than a year now, scientists have been racing to grasp how the mysterious new virus that causes COVID-19 damages not solely our bodies, but in addition our brains.
Early within the pandemic, some contaminated individuals observed a curious symptom: the lack of scent. Reports of different brain-related signs adopted: complications, confusion, hallucinations, and delirium. Some infections have been accompanied by melancholy, anxiousness, and sleep issues.
Recent research recommends that leaky blood vessels and irritation are one way or the other concerned in these signs. But many fundamental questions stay unanswered concerning the virus, which has contaminated more than 145 million individuals worldwide. Researchers are nonetheless attempting to determine how many individuals expertise these psychiatric or neurological issues, who are most in danger, and the way lengthy such signs may final. And details stay unclear about how the pandemic-causing virus, referred to as SARS-CoV-2, exerts its results.
Getting the numbers“
We nonetheless haven’t established what this virus does within the mind,” says Elyse Singer, a neurologist at the University of California, Los Angeles. There are most likely many solutions, she says. “It’s going to take us years to tease this apart.”
For now, some scientists are specializing in the fundamentals, together with how many individuals expertise these types of brain-related issues after COVID-19.
Current research of digital well-being data reported an alarming reply: In the six months after infection, one in three people had experienced a psychiatric or neurological diagnosis. That consequence, printed April 6 in Lancet Psychiatry, got here from the well-being data of more than 236,000 COVID-19 survivors. Researchers counted diagnoses of 14 problems, starting from psychological sicknesses similar to anxiousness or melancholy to neurological occasions similar to strokes or mind bleeds, within the six months after COVID-19 an infection.
“We didn’t expect it to be such a high number,” says research co-author Maxime Taquet of the University of Oxford in England. One in three “might sound scary,” he says. But it’s not clear whether or not the virus itself causes these problems instantly.
The overwhelming majority of these diagnoses have been melancholy and anxiousness, “disorders that are extremely common in the general population already,” factors out Jonathan Rogers, a psychiatrist at University College London. What’s more, melancholy and anxiousness are on the rise amongst everybody in the course of the pandemic, not simply individuals contaminated with the virus.
Mental well-being problems are “extremely important things to address,” says Allison Navis, a neurologist on the post-COVID clinic at Icahn School of Medicine at Mount Sinai in New York City. “But they’re very different than a stroke or dementia,” she says.
About 1 in 50 individuals with COVID-19 had a stroke, Taquet and colleagues discovered. Among individuals with extreme infections that got here with delirium or different altered psychological states, although, the incidence was a lot increased — 1 in 11 had strokes.
Taquet’s research comes with caveats. It was a glance again at prognosis codes, typically entered by hurried clinicians. Those aren’t at all times dependable. And the research finds a relationship, however can’t conclude that COVID-19 precipitated any of the diagnoses. Still, the outcomes trace how COVID-19 impacts the mind.
Blood vessels scrutinized
Early on within the pandemic, the lack of scent recommended that the virus may be capable to assault nerve cells instantly. Perhaps SARS-CoV-2 may breach the cranium by climbing alongside the olfactory nerve, which carries smells from the nostril onto the mind, some researchers thought.
That scary state of affairs doesn’t appear to occur a lot. Most research thus far has failed to show up a lot of virus within the mind, if any, says Avindra Nath, a neurologist who researches central nervous system infections on the National Institutes of Health in Bethesda, Md. Nath and his colleagues anticipated seeing indicators of the virus in the brains of individuals with COVID-19 however didn’t discover it. “I kept telling our folks, ‘Let’s go look again,’” Nath says.
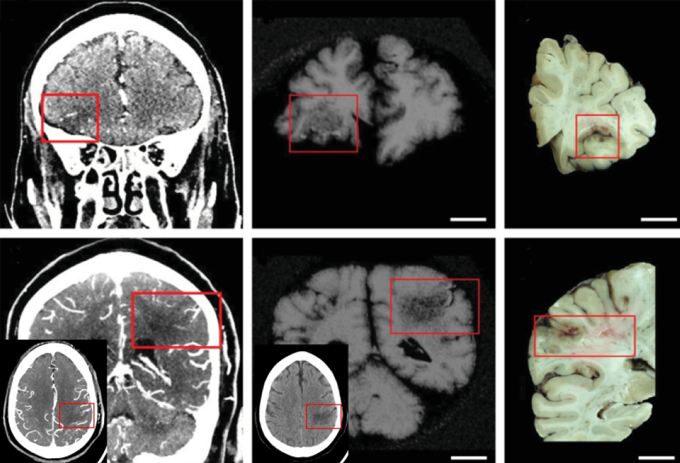
That absence means that the virus is affecting the mind in different methods, presumably involving blood vessels. So Nath and his workforce scanned blood vessels in post-mortem brains of people that had been contaminated with the virus with an MRI machine so highly effective that it’s not accredited for medical use in dwelling individuals. “We were able to look at the blood vessels in a way that nobody could,” he says.
Damage abounded, the workforce reported February 4 within the New England Journal of Medicine. Small clots sat in blood vessels. The partitions of some vessels have been unusually thick and infected. And blood was leaking out of the vessels into the encompassing mind tissue. “You can see all three things happening at the same time,” Nath says.
Those outcomes recommend that clots, infected linings, and leaks within the boundaries that usually preserve blood and different dangerous substances out of the mind could all contribute to COVID-related mind injury.
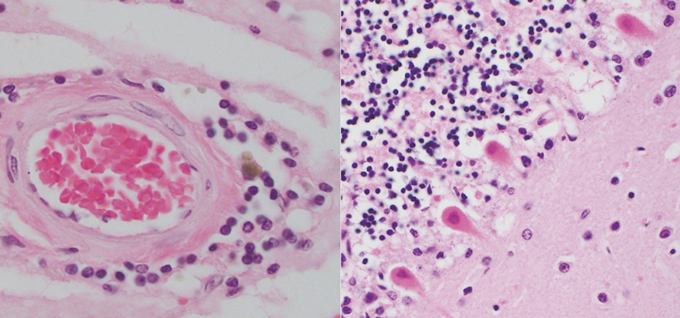
But several unknowns forestall any particular conclusions about how these broken blood vessels relate to individuals’ signs or outcomes. There’s not a lot of medical info out there concerning the individuals in Nath’s research. Some seemingly died from causes apart from COVID-19, and nobody is aware of how the virus would have affected them had they not died.
Inflamed physique and mind
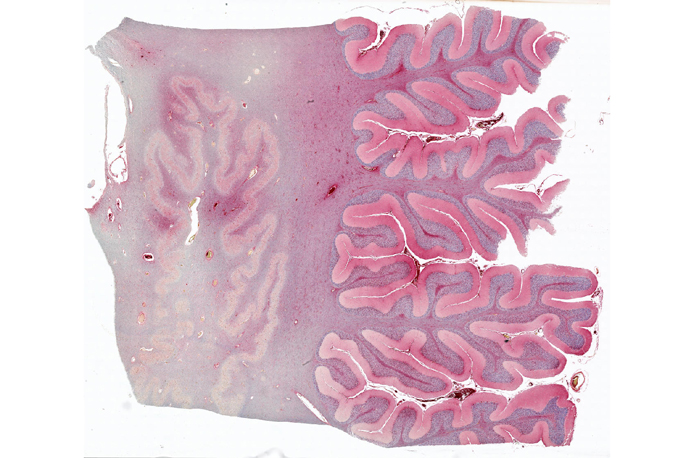
Inflammation within the physique could cause hassle within the mind, too, says Maura Boldrini, a psychiatrist at Columbia University in New York. Inflammatory indicators launched after damage can change the best way the mind makes and makes use of chemical signaling molecules, referred to as neurotransmitters, that assist nerve cells to talk. Key communication molecules similar to serotonin, norepinephrine, and dopamine can get scrambled when there’s a lot of irritation.
Neural messages can get interrupted in individuals who endure traumatic mind accidents, for instance; researchers have discovered a relationship between irritation and psychological sickness in soccer gamers and others who skilled hits to the top.
Similar proof comes from individuals with melancholy, says Emily Troyer, a psychiatrist at the University of California, San Diego. Some individuals with melancholy have excessive ranges of irritation, research has discovered. “We don’t actually know that that’s going on in COVID,” she cautions. “We just know that COVID causes inflammation, and inflammation has the potential to disrupt neurotransmission, particularly in the case of depression.”
Among the cells that launch inflammatory proteins within the mind are microglia, the mind’s model of the physique’s disease-fighting immune system. Microglia might also be concerned with the mind’s response to COVID-19. Microglia primed for action have been present in about 43 % of 184 COVID-19 sufferers, Singer and others reported in an evaluation printed February 4 in Free Neuropathology. Similar outcomes come from a collection of autopsies of COVID-19 sufferers’ brains; 34 of 41 brains contained activated microglia, researchers from Columbia University Irving Medical Center and New York-Presbyterian Hospital reported April 15 in Brain.
With these findings, it’s not clear that SARS-CoV-2 impacts individuals’ brains in a different way from different viruses, says Navis. In her post–COVID-19 clinic at Mount Sinai, she sees sufferers with fatigue, complications, numbness, and dizziness — signs which are identified to observe different viral infections, too. “I’m hesitant to say this is unique to COVID,” Navis says. “We’re just not used to seeing so many people getting one specific infection, or knowing what the viral infection is.”
Teasing aside all of the methods the mind can endure amid this pandemic, and the way that impacts any given individual is unattainable. Depression and anxiousness are on the rise, surveys recommend. That rise may be particularly sharp in individuals who endured tense diagnoses, sicknesses, and isolation.
Just being in an intensive care unit can confuse. Delirium affected 606 of 821 individuals — 74 % — whereas sufferers have been in intensive care items for respiratory failure and different critical emergencies, a 2013 research discovered. Post-traumatic stress dysfunction troubled about a third of people who had been seriously sick with COVID-19 (SN: 3/12/21).
More particular points of remedy matter too. COVID-19 sufferers who spent lengthy intervals of time on their stomachs may need lingering nerve ache, not as a result of the virus attacked the nerve, however, as a result of the susceptible place compressed the nerves. And individuals may really feel mentally fuzzy, not due to the virus itself, however as a result of a scarcity of the anesthetic drug, propofol, meant they obtained an alternate sedative that may carry more aftereffects, says Rogers, the psychiatrist at University College London.
Lingering questions — what the virus truly does to the mind, who will endure essentially the most, and for a way lengthy — are nonetheless unanswered, and doubtless gained’t be for a very long time. The various and damaging results of lockdowns, the imprecision medical doctors and sufferers use for describing signs (such because the nonmedical time period “brain fog”), and the oblique results the virus can have on the mind all merge, making a devilishly complicated puzzle.
For now, medical doctors are busy specializing in methods wherein they may also help, even amid these mysteries, and designing bigger, longer research to raised perceive the consequences of the virus on the mind. That info shall be key to serving individuals transfer ahead. “This isn’t going to be over soon, unfortunately,” Troyer says.
Source
Check below for more similar opportunities:
Patterns in brain activity can identify who will struggle to read(Opens in a new browser tab)
Explainer: What is a neuron?(Opens in a new browser tab)




